Five Tips to Improve Your Golf Game and Avoid Injury
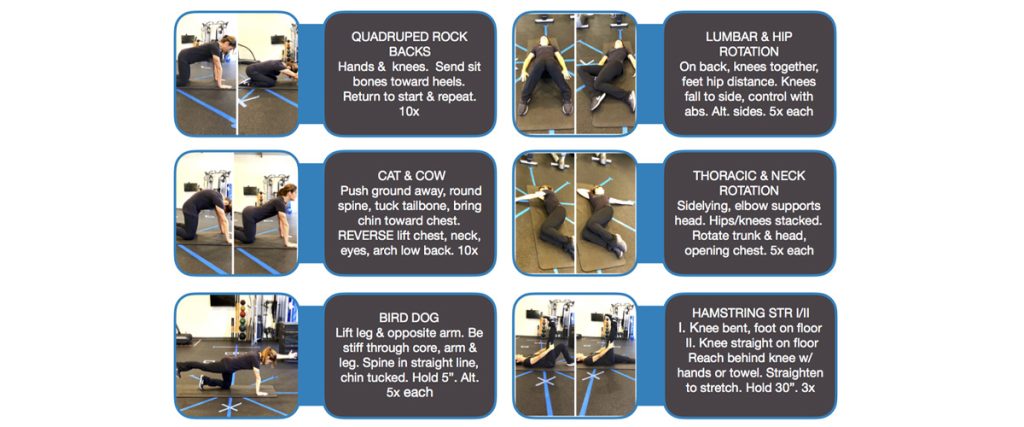
“Jack Nicklaus had it right when he said, ‘Professional golfers condition to play golf; amateur golfers play golf to condition.’ That explains why 62 percent of amateurs will sustain a significant golf injury, typically because they’re out of shape, have poor swing mechanics, or don’t adequately warm up.” -Dr. James Andrews Like in many sports, golf requires complex, multi-dimensional movement, particularly during its golf swing. During the golf swing, the body acts as a kinetic chain and needs its parts to work in tandem. If any part of the chain is lacking, other parts of the body will start to compensate. This can lead to bad habits developing and possible injury in the future. Common swing faults manifest as poor form during backswing, downswing, or follow through. Some common problems can include deficits in balance and posture, and decreased mobility of the hips, mid-back, shoulder blades, or neck. Joint restrictions, muscle tightness, or poor body mechanics can also contribute to compensatory movements during execution of the golf swing. Here are FIVE TIPS to help you to improve your golf game and decrease risk of injury: Warm up – perform a golf-specific warm up that includes trunk rotation and static and dynamic stretching of the major golf muscles, including the shoulders, low back, hamstrings, chest, and wrists. One research article showed that the group that performed this warm up routine demonstrated improvements in club head speed compared to the control group1 Strength train the right muscles – research is showing that training the leg-hip, trunk power, and grip strength are especially relevant for golf performance improvement2 Take breaks – a systematic review found that the higher the frequency of swing repetitions, the greater the cumulative load on the low back. Maintain your back health by gradually building up your golf swing volume3 Double Strap – if you are carrying your own golf clubs, make sure to invest in a bag that has two straps like a backpack. A single strap golf bag places more stress on the shoulder it is placed on Get evaluated – get your golf swing checked out by a professional to make sure you are not developing bad swing habits that will predispose you to future injury A licensed physical therapist can provide a golf-specific program and guide you through exercises specifically designed to: Improve the flexibility of your shoulder and hip musculature. Limited flexibility can affect your backswing and follow through position. Improve mobility of your joints, including the hip, low back, mid back, shoulder, and neck. Limited joint mobility can affect your swing mechanics due to compensations Improve glute and core strength for efficient power development and transfer of energy from your hips, up through your trunk and arms, and into the golf club Improve dynamic balance through hip and abdominal control to maintain proper body mechanics throughout the golf swing At Elevate Physical Therapy & Fitness, our Doctors of Physical Therapy can help you recover from any golf-related injuries, as well as improve your golf game performance. We will assess your biomechanics and ensure proper range-of-motion and strength to achieve optimal golf swing mechanics. We can also create a treatment or fitness plan to address any deficits that are impacting your golf game to help you play at your best! Whether you play golf for a living or just a few times a year, physical therapy can help to prevent golf-related injuries and promote optimal fitness to improve your golf performance. Through the months of January & February we will be posting weekly practical tips and tests on Instagram to help with your golf swing. Check us out @elevateptfit! Stay healthy. Stay well. Stay active. References Fradkin A. Improving golf performance with a warm up conditioning programme. Br J Sports Med. 2004;38(6):762-765. doi:10.1136/bjsm.2003.009399 Torres-Ronda L, Sanchez-Medina L, Gonzalez-Badillo J. Muscle Strength and Golf Performance: A Critical Review. J Sports Sci Med. 2011;10(1):9-18. M. Lindsay D, A. Vandervoort A. Golf-Related Low Back Pain: A Review of Causative Factors and Prevention Strategies. Asian J Sports Med. 2014;5(4). doi:10.5812/asjsm.24289